Workforce
Deploy AI Employees and Scale Your Team Faster
42 AI agents across 7 industries that deliver real business impact.
Workforce
42 AI agents across 7 industries that deliver real business impact.


An AI medical scribe is an AI-powered solution that listens to patient and clinician conversations during visits and automatically generates structured SOAP notes in seconds. Bitontree's AI medical scribe captures every clinical encounter, transcribes it accurately, and converts it into properly formatted SOAP notes integrated with your EHR. The platform saves 90% of documentation time, reduces errors from rushed charting, and lets clinicians focus on patient care instead of paperwork.
How it works
The process starts by securely recording patient-clinician conversations made during a visit. The conversation is then transcribed by our AI medical scribe and automatically structured into accurate SOAP notes. Clinicians can easily review, edit as needed, and finalize their notes with confidence. This simple three-step approach minimizes the workload on documentation and is easily integrated into routine clinical practice.
With a single click, securely capture the entire doctor-patient conversation in real time, ensuring nothing important is missed.
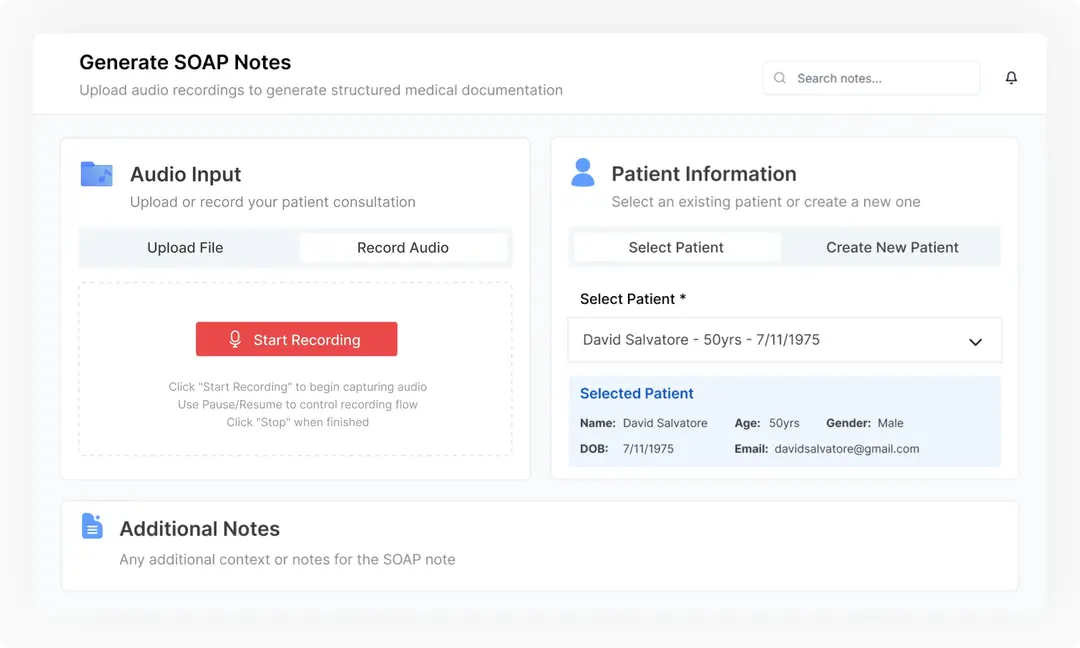
Our AI automatically transcribes the conversation and generates a structured SOAP note, complete with accurate summaries of symptoms, assessments, and plans.
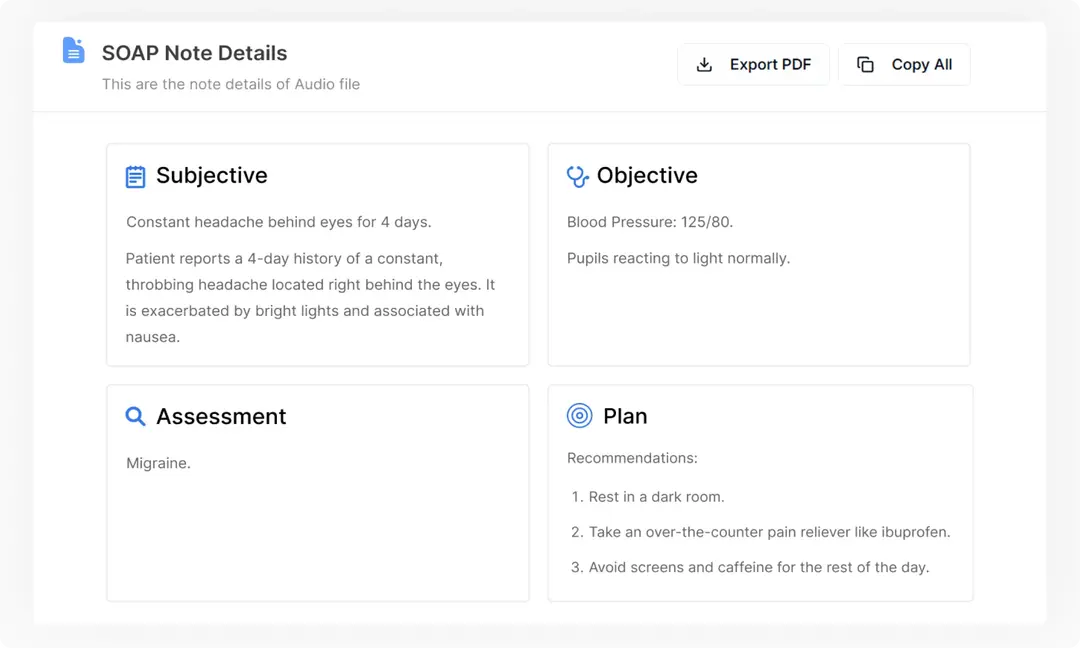
Easily review the draft note, make quick edits if needed, and approve a polished version ready for your medical records.
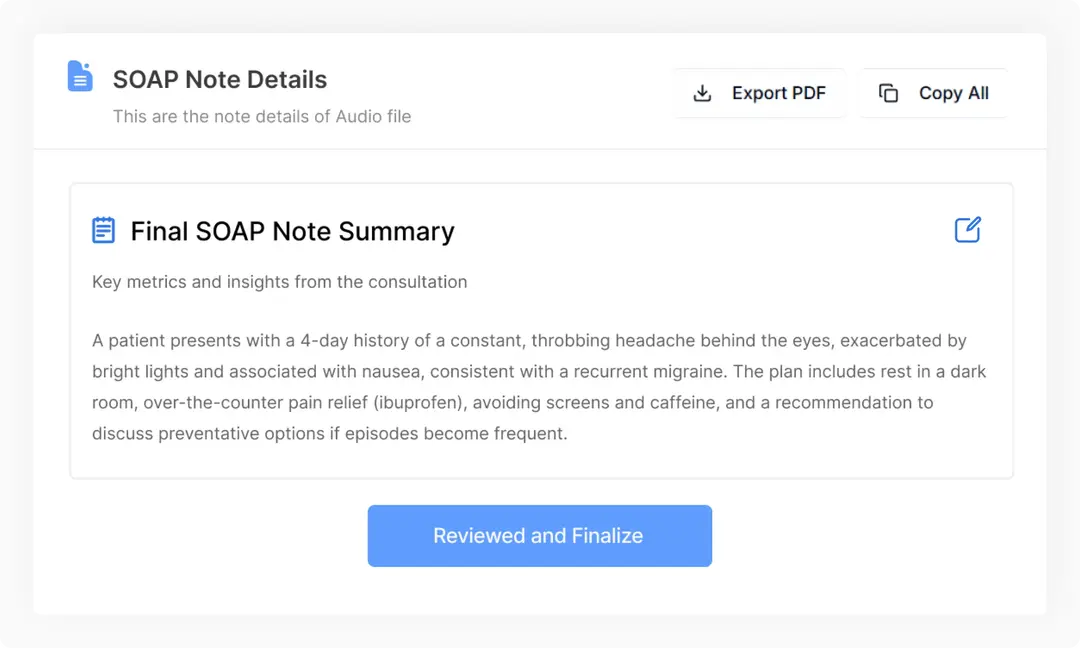
AI-driven SOAP note automation transcribes clinician-patient conversations into structured, high quality and accurate SOAP notes. Decrease in paperwork caused by rapid documentation and the use of a standard note format enhances clinic productivity. As clinicians are interrupted less during visits, they are able to concentrate more on the patient and less on their documentation. This AI clinical documentation leads to seamless daily operations, reduced burnout, and better continuity of care across the practice.
weekly on documentation through automated SOAP notes.
with lower admin load and more focus on patient care.
of reports and biomarkers for improved long-term care.
Key Features
AI SOAP Notes makes clinical documentation easy by transforming patient conversations into precise and structured notes. These intelligent features minimize manual paper work, automate routine activities and guarantee standardized and error-free clinical documentation. Clear, context-aware notes help clinicians make quicker, more informed decisions while staying fully engaged with patients.
Automatically delivers AI SOAP notes via structured data from voice, EHR systems or manual text input to effortlessly document each patient visit while reducing manual charting and time spent by clinicians.
Safely captures doctor-patient conversations in real-time for immediate note generation. This AI medical scribe feature allows clinicians to simply "be present" with patients without worrying about documentation burden.
Smart EHR integration allows seamless import and export of patient information and generated notes directly within existing EHR systems. This removes duplicate data entry while ensuring clinical workflows can continually receive information on cases.
AI understands clinical context and automatically organizes conversations into Subjective, Objective, Assessment, and Plan sections. This SOAP notes automation ensures structured, specialty-aligned clinical notes that are consistent, accurate, and ready for review without additional formatting.
Transcribes consultation audio uploaded or recorded by the user into precise medical documentation. This allows clinicians to capture encounters the way they wish while maintaining consistency in records.
Provides a unified view of generated notes, patient activity, and efficiency of metrics onto a single dashboard. This helps practice track performance, streamline workflows, and measure documentation impact.
Whom we serve
Our Automated SOAP Note solution is designed to support a wide range of care settings and practice sizes, from solo providers to large healthcare organizations. It delivers consistent, reliable and high-quality documentation regardless of visit volume or complexity. Whether in a solo practice or large clinic, providers can trust that this SOAP notes software for clinics will help create better care and run an efficient business.
Built for solo practitioners and small practices, the AI SOAP Note solution reduces time on documentation and paperwork. This AI medical documentation tool allows clinicians to spend more time with patients while maintaining accurate and compliant records.
Enterprise grade transcription is designed for high-volume clinical setting and enables streamlined, consistent, and standardized documentation of patient health information. Our AI clinical documentation workflows from AI make it easier to be more efficient, compliant and coordinate across departments.
Easily and safely integrate AI SOAP note transcription to your EHR, enabling direct access to structured notes and preserving the value you offer customers without disrupting their experience. This automated SOAP notes integration ensures seamless connectivity.
Support high-volume specialties like urgent care, cardiology or pediatrics by producing structured notes that meet specialty-specific documentation requirements and improves clinical decision-making. Our SOAP notes software for clinics adapts to diverse specialty needs.
Discover what our clients say about working with us and how we’ve contributed to their success.
Our AI-powered transcription is highly accurate, capturing medical terminology, abbreviations, and context-specific information. Accuracy improves over time as it adapts to your practice’s language and workflow.
Yes. Our solution is designed to integrate easily with most major EHR systems and health software platforms, enabling seamless workflow without disrupting your existing clinical operations.
Absolutely. By automating up to 90% of the documentation process, providers spend less time on paperwork and more time on patient care, improving job satisfaction and reducing stress.
Our AI is trained on medical terminology across multiple specialties. It accurately interprets complex terms, abbreviations, and context-specific language to produce precise and reliable SOAP notes.
The AI helps generate structured practice relevant notes, but clinicians always retain full control. Our AI medical scribe notes can be previewed, edited and completed prior to saving for accuracy and clinical confidence.
The platform follows healthcare-grade security measures such as data encryption, secure storage and access controls. Our SOAP notes automation is designed to meet HIPAA and other compliance requirements for the protection of patient privacy.
Implementation is quick and easy. Most practices can be onboarded within few days, including setup, EHR integration, and basic training without interruption to everyday workflow.
Yes. The AI adapts to specialty-specific terminology, note structures, and clinical workflows, making it suitable for practices such as primary care, pediatrics, cardiology, behavioral health, and more.